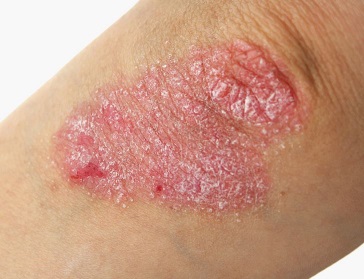
Psoriasis is a chronic inflammatory skin condition characterised by red and scaly plaque rash. It is thought to be immune-mediated inflammatory (autoimmune) disease. It is not contagious. Psoriasis also can affect nails and joints (causing psoriatic arthritis). Psoriasis affects 2-4% of males and females. It affects at any age from childhood to adult. It has peaks onset of 30-39 years and 50-69 years.
Risk factor for triggering or worsening psoriasis:
- Family history especially in those with first degree relatives. Genetics suspectibility with major histocompatibility complex on chromosome 6p21, IL-12 and IL-23 genes had been implicated in psoriasis
- Smoking
- Obesity
- Drugs such as Lithium, Beta- blockers, antimalarials, nonsteroidal anti-inflammatory drugs
- Infections due to viral or bacterial infections. Poststreptococcal infection causes flare of guttate psoriasis. HIV is known to worsen the condition of psoriasis.
- Excess alcohol consumption
Clinical features:
Psoriasis usually presents with symmetrically distributed, red, scaly plaques with well defined borders. The scale can be silvery white and may have peeling surface. Scaling and redness of skin occurs due to increased growth than normal and cells turnover in psoriasis with inflammation. In normal skin, the skin cells turnover is 27 days but in psoriasis, the skin cells turnover become shortened to 4 days. The most common sites affected are scalp, elbows and knees. In severe form of psoriasis, it can affect the whole body. Some patient can complain itchy of the skin leading to scratching and lichenification (thickened leathery skin).
Types of psoriasis:
- Chronic plaque psoriasis- most common psoriatic rash and symmetrically distributed plaques on the scalp, extensor elbows, knees and back
- Guttate psoriasis- sudden eruption of multiple small psoriatic papules and plaques usually after streptococcal throat infection
- Pustular psoriasis- can have life-threatening complications such as renal, hepatic or respiratory abnormalities. There is usually acute onset of widespread rash with scaling and pustules. It can be associated with general unwell, fever, diarrhoea, elevated white cell counts and low calcium.
- Erythrodermic psoriasis- may be acute or chronic with generalised erythema and scaling from head to toe. May result in temperature dysregulation, electrolyte imbalance and cardiac failure. Admission to hospital may be necessary.
- Inverse psoriasis- involving groin areas, buttock, armpits and under breast areas
- Nail psoriasis- pitting
- Scalp psoriasis- often the first or only site of psoriasis
Health conditions associated with psoriasis:
- Psoriatic arthritis- arthritis and inflammation of tendons involving fingers and toes
- Metabolic syndrome- obesity, high blood pressure, high cholesterol, gout, cardiovascular disease and Type 2 diabetes mellitus
- Eye involvement- inflammation of eyelids, eye and and conjunctivitis
Diagnosis:
Psoriasis is diagnosed by its clinical features. If necessary, skin biopsy can be taken to confirm the diagnosis.
Treatment:
Depending on the severity of psoriasis and patient's choice, treatment will be tailored based on individual's need. Mild psoriasis which only involved small area of skin can be treated with topical treatment only.
Topical treatments
- cortisone cream
- Daivobet cream
- coal tar (for scalp psoriasis)
Moderate to severe psoriasis with involvement of 5% to 10% of the body surface or involvement of face, palm of hand or sole of foot are generally treated with phototherapy or systemic therapy since topical treatment is not practical. Phototherapy with ultraviolet radiation is used to treat psoriasis.
Systemic treatments
- Methotrexate- known to be successfully treated psoriasis for more than three decades. Less effective than biologic therapies. This is usually dosed once weekly.
- Cyclosporine- immunosuppresant agent. Comparable to Methotrexate. Used in erythrodermic psoriasis. It requires monitoring of kidney function and blood pressure.
- Acitretin- vitamin A derivatives. Works very well in pustular and erythrodermic psoriasis. It requires monitoring of liver function test and cholesterol level. Pregnancy is contraindicated during the treatment and for 3 years after discontinuining the drug.
- Apremilast- new drug released in 2014. Does not work as effective as biologic therapies. Side effects are headache, diarrhoea, nausea, upper respiratory tract infection and weight loss.
- Biologic therapies such as Etanercept, Infliximab, Adalimumab, Ustekinumab, Secukinumab, Ixekizumab, Brodalumab, Alefacept (only dermatologists can prescribe). Infliximab works faster and more effective among others. It is given in intravenous infusion.
Future therapies (still in research)
- Therapies targeting the Th17 pathway
- Small molecules- Janus kinase and protein kinase C inhibitor. The drug is given orally. Research so far show very promising result.